
Remember the first time you ever saw an ultrasound machine? Boy, I sure do! It was an Acuson 128xp at the University of Florida Veterinary School in the early 90’s.. It was this giant rectangle on wheels that weighed a ton, had a little tv on the top that made pretty images of snowstorms (on film!), and had so many knobs and buttons on it that it looked like it came straight out of the NASA command center.
I would sit on the opposite side of the table holding the patient and watch the radiologist turn those knobs and push those buttons and try to make some sense of all that twinkly madness! “This is a nodule in the liver” the radiologist would say…sure it is…(just smile and nod…) And when we had to do horse tendons in the barn I really got a work out trying to move that behemoth and lost a few years off my life worrying that something would happen to it while I was wheeling it around. I mean, look at this monster!! Ultrasound machines sure have come a long way (thank goodness)!
There are a lot of knobs and buttons on ultrasound machines and rest assured they all do something just in case you were wondering if they were just for show. It makes sense that there has to be a way to control the sound frequencies and change the image around so we can actually make some sense of it all.
Now all machines are not created equal in that the knobs and buttons are not always in the same place and one system’s knob is another system’s button. Luckily though the functions of the knob/buttons are the same on most every machine. I have to be a little bit more “techy” for this part. There is no way around it but I did my best to keep it as simple as possible.

Here we go. Let’s start with the knobs/buttons and adjustments that you should be using for every exam. When we are done go to your own machine and locate them! They are as follows:
- On/off switch – you laugh but, in a lot of clinics that amazing technician that you have does this for you every morning and night so you don’t have to worry about it. It is a good idea to know where it is so just in case something goes awry and it locks up and you have to reboot.
- Probe change(switch) button – making sure you have the correct probe especially if you have more than one.
- Frequency – The highest frequency on the multi-frequency transducer should be used first and adjusted as needed. You should know the limits of your transducer’s highest and lowest frequency setting.Ultrasound frequencies range from 2 MHz to approximately 15 MHz. It is important to remember that higher frequencies of ultrasound have shorter wavelengths and are absorbed/attenuated more easily. Therefore, higher frequencies are not as penetrating. This explains why high frequencies are used for the superficial body structures and low frequencies are used for those that are deeper. Ultrasound transducers contain more than one operating frequency.The following frequencies are a guide to frequencies typically used for ultrasound examination:
- 2.5 MHz: deep abdomen
- 3.5 MHz: general abdomen
- 5.0 MHz: vascular
- 7.5 MHz: thyroid
- 10.0 MHz: thyroid, superficial veins, superficial masses, musculoskeletal imaging
- 15.0 MHz: superficial structures, musculoskeletal imaging
- Depth/Focal zone adjustment – These two functions go hand in hand. You change the depth to bring the area of interest into the near or far field and once you do that you change the focal zone. The focal zone provides the best detail in the x-direction, as this is the thinnest section of the ultrasound beam. Think of it as the “sweet spot” of the sound wave.Every ultrasound beam (primary) has narrowing at the focal zone and then beam broadening or divergence deep to the focal zone. The focal zone should be set at the level of or just below the area or organ of interest. The focal zone is typically displayed on the image as a triangle or arrow head that can be moved from near to far field and back again.


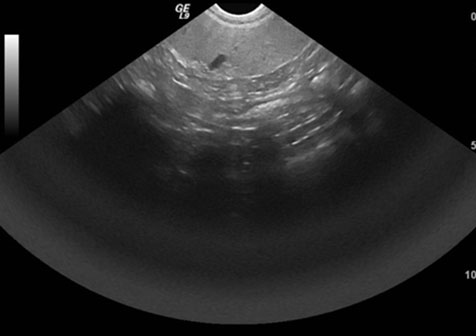
-
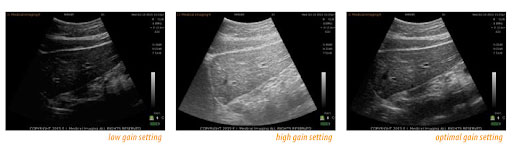
Gain and TGC (time gain compensation usually knob and sliders) – used to help adjust the overall image brightness. Remember that this is a post processing technique that basically increases the overall whiteness of the screen and has nothing to do with the way the ultrasound waves are produced, transmitted or processed.
The overall gain should not be set higher than 70% when optimizing the image. If you have to go higher than 70% then think about decreasing the frequency of the transducer. Remember to scan in a room with low light (NOT DARK OR FULL LIGHTING!) This can have a profound effect on how you set your gain.
When using the TGC, use the mid-range as a starting point. Then adjust the sliders from a straight vertical position to a slight angle with the top slider being more to the left (decreasing the overall gain in the near field) and the bottom slider being more to the right (increasing the overall gain in the far field). This should help with the loss of ultrasound wave numbers at depth within the tissue.

-
Image Contrast Settings (also called log compression or dynamic range) – controls the overall gray scale of the image. A short dynamic range means that the image is black and white with very little gray like an echocardiogram. A long dynamic range there is little contrast and a long gray scale that makes many different shades of gray and subtle lesions could be obscured, so for abdomen mid-dynamic range is preferred.
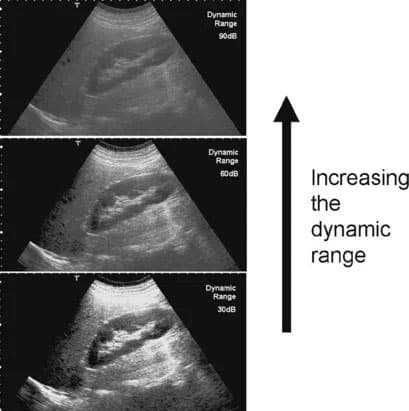
Ready? Let’s go for a drive! Turn on your machine (if that tech hasn’t already done so) and enter the patient information if you are capturing images. If you are using a PACS system you should assign a specific unique medical record number. This will ensure storage of all of the images related to the patient (unique medical record number) will take place and make sure to use it every time you scan this patient.
Depending on your clinical patient management system the ultrasound machine can be populated with patients from that system (AKA- Worklist! This is a question for your friendly Ultrasound Salesperson!!) In addition, a unique accession number will be specific to the actual study number (unique study, individual, date and time) done at the hospital.
After the patient data is entered, choose the specific probe and settings preset for imaging the patient. Most patients will be scanned with the microconvex and if you happen to have a linear transducer use it for cats, small dogs or superficial lesions/structures such as GI.
What is a preset you ask? A preset is a specific combination of knob settings that have been adjusted and set by you when you get the image quality you are happy with. Again, your friendly Ultrasound salesperson or tech support can help you with this for your particular machine! There are factory presets but these are usually changed to the personal preference of the sonographer.
After the preset is chosen, you are ready to scan the patient. Use liberal amounts of ultrasound gel to ensure adequate contact between the transducer and the skin and it is good to have some Isopropyl alcohol around as well just in case you can’t put gel on your patient and it seems to help the gel do its job. A specific sequence of organ and area evaluation should take place (we talked about that in Blog #1).
Whew! That was a long tale not as long as War and Peace, mind you, but long enough!! Image optimization is important and takes some getting used to because there are so many different things to think about with all the knobs. Presets do help because it is a way to set all these knobs but, it pays to know how to manipulate them yourself because not every patient is created equal!!
Best thing? When you start a scan use the liver as your subject and play with all the knobs/buttons. Turn them to their extremes and see what they do. If you mess up your settings, you can always reset them.
Next blog we will discuss those other knobs/buttons that you may/may not use! As always, PRACTICE! PRACTICE! PRACTICE!
